Last reviewed: October 2, 2022
Recommendation:
- If clinicians choose to use ultrasound for medical abortion follow-up, the only ultrasound finding that requires intervention is an ongoing viable pregnancy.
Strength of recommendation: Strong
Quality of evidence: Low
Background
Ultrasound is not necessary to provide abortion care (World Health Organization [WHO], 2014) but may be common in some settings. Ultrasound for follow-up after medical abortion has diagnostic limitations. Except for the case of an ongoing viable pregnancy, intervention after a medical abortion should be based on clinical symptoms and not ultrasound findings.
Ultrasound findings at follow-up
Endometrial thickening
After a successful medical abortion, endometrial thickness varies and can be associated with a complex or heterogeneous appearance.
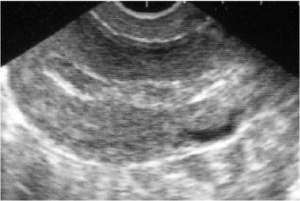
Endometrial thickening
Courtesy of Mary Fjerstad
A 2021 systematic scoping review, which included 79 randomized controlled trials and 169 observational studies, examined criteria for diagnosing retained products of conception following induced or spontaneous abortion before 14 weeks gestation, finding that although most studies utilized ultrasound, there was little diagnostic accuracy of this method (Hamel et al., 2021). Multiple retrospective and prospective cohort studies have shown that endometrial thickness ranges widely in women after medical abortion, with significant overlap between women with successful and failed medical abortion (Cowett et al., 2004; Markovitch et al., 2006; Parashar et al., 2007; Rørbye, Nørgaard, & Nilas, 2004; Tzeng et al., 2013). In a pooled analysis of 2,208 women one week after medical abortion, after women with a persistent gestational sac were excluded, the average endometrial thickness was 10.9mm in women who did not require more intervention and 14.5mm in 30 women who did require intervention (Reeves et al., 2009). Although the average endometrial thickness in women who require intervention tends to be higher, because of the range and overlap between successful and unsuccessful abortion, no study has found that there is a thickness above which a diagnosis of unsuccessful medical abortion can be made. The decision to intervene should be made on clinical signs and symptoms, such as ongoing or heavy bleeding, rather than on ultrasound findings.
Persistent gestational sac
A persistent gestational sac, in which the sac is present but there is no viable embryonic tissue, occurs in less than 1% of medical abortions with the recommended mifepristone and misoprostol regimen (Creinin et al., 2004; Creinin et al., 2007; Winikoff et al., 2008). A persistent gestational sac is not a viable pregnancy and may be managed with aspiration, a second dose of misoprostol or expectant management according to a woman’s preference. In a study of women with a persistent gestational sac within 11 days of medical abortion, a second dose of misoprostol was found to lead to expulsion in 69% of women (Reeves, Kudva, & Creinin, 2008).
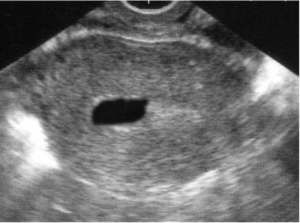
Persistent gestational sac: Courtesy of Mary Fjerstad
Ongoing viable pregnancy
An ongoing pregnancy, in which a growing sac and/or embryo with cardiac activity are present, occurs in less than 1% of medical abortions with the recommended mifepristone and misoprostol regimen (Chen & Creinin, 2015; Von Hertzen et al., 2009; Winikoff et al., 2008). Some women will be able to identify this outcome without ultrasound due to lack of bleeding or continued pregnancy symptoms. A woman with an ongoing pregnancy should be offered uterine evacuation as soon as possible with either vacuum aspiration or a second dose of misoprostol, depending on gestational age and local context. The success rate of misoprostol after failed medical abortion is 36% (Reeves et al., 2008). If a woman chooses a second dose of misoprostol, she must be followed to see if it is successful.
References
Cowett, A. A., Cohen, L. S., Lichtenberg, E. S., & Stika, C. S. (2004). Ultrasound evaluation of the endometrium after medical termination of pregnancy. Obstetrics & Gynecology, 103(5, Part 1), 871-875.
Chen, M. J., & Creinin, M. D. (2015). Mifepristone with buccal misoprostol for medical abortion: A systematic review. Obstetrics & Gynecology, 126(1), 12-21.
Creinin, M. D., Fox, M. C., Teal, S., Chen, A., Schaff, E. A., & Meyn, L. A. (2004). A randomized comparison of misoprostol 6 to 8 hours versus 24 hours after mifepristone for abortion. Obstetrics & Gynecology, 103(5, Part 1), 851-859.
Creinin, M. D., Schreiber, C. A., Bednarek, P., Lintu, H., Wagner, M. S., & Meyn, L. A. (2007). Mifepristone and misoprostol administered simultaneously versus 24 hours apart for abortion: A randomized controlled trial. Obstetrics & Gynecology, 109(4), 885-894.
Hamel, C.C., van Wessel, S., Carnegy, A., Coppus, S.F.P.J., Snijders, M.P.L., Clark, J., & Emanuel, M.H. (2021). Diagnostic criteria for retained products of conception-A scoping review. Acta Obstetricia et Gynecologia Scandinavica 100(12), 2135-2143.
Markovitch, O., Tepper, R., Klein, Z., Fishman, A., & Aviram, R. (2006). Sonographic appearance of the uterine cavity following administration of mifepristone and misoprostol for termination of pregnancy. Journal of Clinical Ultrasound, 34(6), 278-282.
Parashar, P., Iversen, O. E., Midbøe, G., Myking, O., & Bjørge, L. (2007). Medical abortion in the first trimester: The use of serum hCG and endometrial thickness as markers of completeness. European Journal of Contraception and Reproductive Health Care, 12(4), 366-371.
Reeves, M., Fox, M., Lohr, P., & Creinin, M. (2009). Endometrial thickness following medical abortion is not predictive of subsequent surgical intervention. Ultrasound in Obstetrics & Gynecology, 34(1), 104-109.
Reeves, M. F., Kudva, A., & Creinin, M. D. (2008). Medical abortion outcomes after a second dose of misoprostol for persistent gestational sac. Contraception, 78(4), 332-335.
Rørbye, C., Nørgaard, M., & Nilas, L. (2004). Prediction of late failure after medical abortion from serial β‐hCG measurements and ultrasonography. Human Reproduction, 19(1), 85-89.
Tzeng, C.R., Hwang, J.L., Au, H.K., & Chien, L.W. (2013). Sonographic patterns of the endometrium in assessment of medical abortion outcomes. Contraception, 88(1), 153-9.
Von Hertzen, H., Piaggio, G., Wojdyla, D., Marions, L., My Huong, N., Tang, O., & Mittal, S. (2009). Two mifepristone doses and two intervals of misoprostol administration for termination of early pregnancy: A randomised factorial controlled equivalence trial. BJOG: An International Journal of Obstetrics & Gynaecology, 116(3), 381-389.
Winikoff, B., Dzuba, I. G., Creinin, M. D., Crowden, W. A., Goldberg, A. B., Gonzales, J., . . . & Shannon, C. S. (2008). Two distinct oral routes of misoprostol in mifepristone medical abortion: A randomized controlled trial. Obstetrics & Gynecology, 112(6), 1303-1310.
World Health Organization. (2022). Abortion care guideline. Geneva: World Health Organization.
